Hypertrophic Cardiomyopathy Treatment is crucial for managing this condition effectively. Hypertrophic cardiomyopathy (HCM) is a genetic heart disease characterized by the thickening of the heart muscle. This thickening can lead to various complications, including heart failure and arrhythmias. Understanding the treatment options available can greatly enhance the quality of life for those affected.
What is Cardiomyopathy?
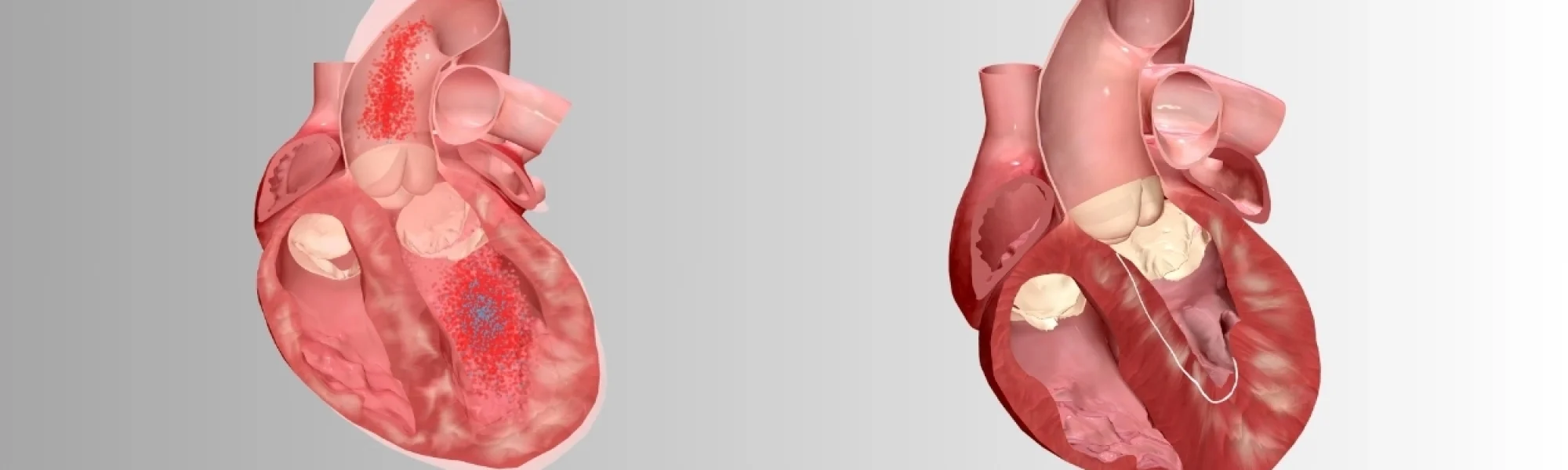
Cardiomyopathy refers to diseases of the heart muscle, where the heart becomes enlarged, thickened, or rigid. There are several types of cardiomyopathy, including hypertrophic, dilated, and restrictive. Hypertrophic cardiomyopathy, specifically, involves the thickening of the heart muscle, particularly the ventricles. This condition can obstruct blood flow and make it harder for the heart to pump effectively, which can lead to serious health issues.
Causes of Hypertrophic Cardiomyopathy
The primary cause of hypertrophic cardiomyopathy is genetic mutations. These mutations affect the proteins in the heart muscle cells, leading to abnormal thickening. Other factors that may contribute include:
- Family history: Many cases are inherited, making family history a significant factor.
- Age: Symptoms may develop over time, particularly in adolescents or young adults.
- Certain medical conditions: Conditions such as high blood pressure can also lead to heart muscle thickening.
Understanding these causes is essential for effective Hypertrophic Cardiomyopathy Treatment.
Stages of Hypertrophic Cardiomyopathy
Hypertrophic cardiomyopathy can be classified into different stages, ranging from mild to severe.
- Mild: Little to no symptoms, with minimal thickening of the heart muscle.
- Moderate: Symptoms may start to appear, including occasional shortness of breath or chest pain during exercise.
- Severe: Significant thickening of the heart muscle, leading to severe symptoms and complications like heart failure or arrhythmias.
Recognizing the stage of the condition is important for determining the appropriate Hypertrophic Cardiomyopathy Treatment.
Side Effects of Hypertrophic Cardiomyopathy
Patients with hypertrophic cardiomyopathy may experience various side effects, including:
- Shortness of breath: Especially during physical activities or exertion.
- Chest pain: Often during exercise or stressful situations.
- Fainting: A sudden loss of consciousness, especially during exertion.
- Arrhythmias: Irregular heartbeats can occur, leading to palpitations or dizziness.
These side effects can significantly impact daily life, making proper Hypertrophic Cardiomyopathy Treatment essential.
Cardiomyopathy Coronary Artery Bypass Surgery
In some cases, patients with hypertrophic cardiomyopathy may require surgical interventions, including coronary artery bypass surgery. This procedure helps improve blood flow to the heart by bypassing blocked arteries. While it’s not a direct treatment for HCM, it can be beneficial for patients who have both HCM and coronary artery disease.
- Purpose: To restore blood flow and reduce symptoms.
- Procedure: Surgeons take blood vessels from other parts of the body and use them to bypass blocked arteries.
- Recovery: The recovery period can vary, but most patients see significant improvements in symptoms.
Understanding this option can help patients explore all avenues for Hypertrophic Cardiomyopathy Treatment.
New Treatments for Hypertrophic Cardiomyopathy
Exciting advancements are being made in the field of hypertrophic cardiomyopathy treatment. Some new treatments include:
- Medications: New drugs targeting specific heart muscle proteins are being studied to reduce thickening.
- Gene therapy: Researchers are exploring ways to modify the genes responsible for HCM.
- Alcohol septal ablation: This procedure involves injecting alcohol into the heart muscle to reduce its thickness.
These new treatments offer hope for better management of hypertrophic cardiomyopathy and can improve patient outcomes significantly.
Signs and Symptoms of Hypertrophic Cardiomyopathy
Recognizing the signs and symptoms of hypertrophic cardiomyopathy is crucial for early diagnosis and treatment. Common symptoms include:
- Shortness of breath: Especially during physical exertion.
- Chest pain: Often felt during exercise or emotional stress.
- Dizziness or fainting: Especially during physical activity.
- Heart palpitations: Feeling an irregular heartbeat or racing heart.
If you or a loved one experience these symptoms, it’s important to consult a healthcare professional for evaluation and potential Hypertrophic Cardiomyopathy Treatment.
Prevention of Hypertrophic Cardiomyopathy
While it may not be possible to prevent hypertrophic cardiomyopathy entirely, certain lifestyle changes can help manage symptoms and reduce risks:
- Regular exercise: Engage in moderate physical activity, as advised by a healthcare provider.
- Healthy diet: Eating a heart-healthy diet can improve overall cardiovascular health.
- Avoiding stimulants: Limit caffeine and avoid illegal drugs that can worsen symptoms.
Implementing these preventive measures can enhance heart health and support Hypertrophic Cardiomyopathy Treatment.
Risks Associated with Hypertrophic Cardiomyopathy
Patients with hypertrophic cardiomyopathy face certain risks, including:
- Heart failure: The heart may struggle to pump effectively.
- Sudden cardiac arrest: This can occur due to severe arrhythmias.
- Increased risk of stroke: Thickened heart muscle can lead to blood clots.
Being aware of these risks allows patients and doctors to work together to implement effective Hypertrophic Cardiomyopathy Treatment plans.
Conclusion
In summary, Hypertrophic Cardiomyopathy Treatment is essential for managing this condition and preventing serious complications. With various treatment options available—from lifestyle changes to advanced cardiomyopathy medical procedure—patients have many avenues to explore. If you or someone you know is dealing with symptoms of hypertrophic cardiomyopathy, don’t hesitate to reach out for more information and personalized care. For further inquiries, feel free to contact us.